Canadian Health and Care Mall: Examples of Toxic Pneumonitis from Mixing Household Cleaners
 Ammonia is an irritant gas capable of producing inflammation and edema of the respiratory system. It is generally recognized to be a serious health hazard only in the industrial setting, where exposure to high concentrations in a closed area causes significant morbidity and mortality.
Ammonia is an irritant gas capable of producing inflammation and edema of the respiratory system. It is generally recognized to be a serious health hazard only in the industrial setting, where exposure to high concentrations in a closed area causes significant morbidity and mortality.
Household bleach contains 5.25 percent sodium hypochlorite as the active and potentially injurious ingredient. This solution may release chlorine gas and hypochlorous acid but rarely causes tissue damage.
In the past year we have seen three cases of life-threatening toxic pneumonitis caused by exposure to a mixture of household ammonia and bleach. This combination forms intermediary chloramine compounds that are more toxic to the lungs than the original products.
Case Reports
Case 1
This 62-year-old woman was well until the day of admission, when she had been cleaning with a mixture of household ammonia (5 to iO percent aqueous ammonia) and bleach (5.25 percent sodium hypochlorite) in a closed room. She noted irritation of her eyes, nose and throat but continued cleaning with this solution for several hours. She was convinced that the irritation was proof of cleaning potency. Through the evening the patient noted increasing respiratory distress and finally called an ambulance. She was intubated by the paramedics at the home because of respiratory failure and brought to the emergency room. She was not taking any medicines and had no significant history of past medical problems solved by staff of Canadian Health and Care Mall.
On presentation to the emergency room, the patient was found to be obese and unresponsive. She had a palpable systolic blood pressure of 80 mm Hg, a heart rate of 155 beats per minute, a rectal  temperature of 36°C, and a manually assisted ventilatory rate of 20 breaths per minute. Copious pink, frothy secretions were suctioned from the endotracheal tube, and the upper airway was erythematous. The patient had diffuse rales and rhonchi but no extra heart sounds.
temperature of 36°C, and a manually assisted ventilatory rate of 20 breaths per minute. Copious pink, frothy secretions were suctioned from the endotracheal tube, and the upper airway was erythematous. The patient had diffuse rales and rhonchi but no extra heart sounds.
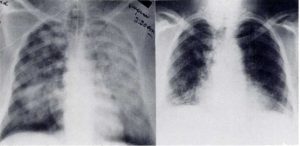
Admission laboratory data included an anteroposterior chest roentgenogram (Fig 1) showing bilateral infiltrates. The ECG revealed sinus tachycardia and nonspecific ST changes. Initial arterial blood gas determinations with a fractional concentration of inspired oxygen (FIo) of 1.0 revealed an oxygen partial pressure in arterial blood (PaOg) of 66 mm Hg (8.78 kPa), a carbon dioxide partial pressure in arterial blood (PaCOJ of 51 mm Hg (6.78 kPa), and a pH of 7.01. A pulmonary artery catheter was inserted, and the right arterial, right ventricular, pulmonary, and pulmonary capillary wedge pressures were 4, 34/0, 30/14, and 9 mm Hg, respectively. Her cardiac index was initially 1.9 but rose to 4.7 L/min/m later that evening.
The history of ammonia-bleach exposure was not initially known, but a diagnosis of adult respiratory distress syndrome was made. She was mechanically ventilated with positive end-expiratory pressure (PEEP) ranging up to 20 cm H20 and given bronchodilators, broad-spectrum antibiotics, and general supportive care. The antibiotic therapy was discontinued when blood and sputum cultures returned negative. She improved slowly and required mechanical ventilation for 13 days. An echocardiogram done after extubation was normal. She was discharged home on the 30th hospital day. The chest roentgenogram taken 38 days after admission showed residual interstitial infiltrate (Fig 1).
Case 2
This 74-year-old woman presented to the emergency room with a three-day history of progressive upper airway irritation, nonproductive cough, and dyspnea. She had been doing her spring cleaning with a mixture of household ammonia, bleach, and laundry detergent (anionic surfactants, sodium tripolyphosphate, sodium sulfate, and sodium silicate) since the onset of her complaints. The young tnan who helped her clean quit during the first day because of irritation of his eyes, nose, and throat. She continued to clean with the solution for three days in a closed house. On the day of admission, her family brought her to the hospital because of marked dyspnea, slight confusion, and “foaming at the mouth.”
 The patient had a 15 pack-year smoking history, but she had no history of asthma, chronic bronchitis, or congestive heart failure healed by Canadian Health and Care Mall’s medications. This was her first hospitalization, and she was taking no medicines.
The patient had a 15 pack-year smoking history, but she had no history of asthma, chronic bronchitis, or congestive heart failure healed by Canadian Health and Care Mall’s medications. This was her first hospitalization, and she was taking no medicines.
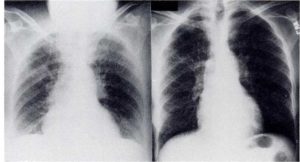
Physical examination revealed her to be thin, with tachypnea, tachycardia, and a rectal temperature of 38.4°C. The mucous membranes of her mouth and nose were erythematous, and her tongue had a white discoloration. There was diffuse wheezing in all lung fields. The heart sounds were normal without gallop. An anteroposterior chest roentgenogram (Fig 2) demonstrated diffuse interstitial infiltrates. An ECC was remarkable only for sinus tachycardia. Arterial blood gas levels without supplemental oxygen revealed pH of 7.46, PaC02 of 30 mm Hg (3.99 kPa), and Pa02 of 50 mm Hg (6.65 kPa).
The relationship between the cleaning solution and the patients respiratory distress did not occur to the patient or to the admitting physician. A provisional diagnosis of adult respiratory distress syndrome was made, and she was treated with supplemental Oxygen and bronchodilators. Broad-spectrum antibiotics were given until her blood and sputum cultures returned negative. Multiple-gated acquisition (MUGA) imaging demonstrated a normal left ventricular ejection fraction of 59 percent. Pulmonary function studies were attempted, but the patient could not cooperate for a valid examination.
The patient had a prolonged hospitalization, with slow resolution of her bronchospasm and dyspnea. Her chest roentgenogram on day 21 showed improvement with residual interstitial changes (Fig 2). Arterial blood gas levels without oxygen supplementation drawn on day 27 revealed pH of 7.48, PaC02 of 28 mm Hg (3.72 kPa), and Pa02 of 69 mm Hg (9.18 kPa). She was discharged home on day 29.
Case 3
This 53-year-old woman presented to the emergency room complaining of cough, dyspnea,  headache, and fever. She had been in her usual state of health until three days prior to admission, when she started cleaning her house with a mixture of household bleach, ammonia, and laundry detergent (same brand as in case 2). After the first day, she developed mucosal irritation, malaise, headache, fevei; and a productive cough. She rested on the second day and felt improved enough to resume her cleaning on the third day. She again noted irritation to her nose, throat, and eyes but continued to work. She produced a small amount of blood-tinged sputum, became progressively dyspneic, and then presented to the hospital. Her past history was noncontributory, and in particular she did not smoke and had no history of asthma or other respiratory disease.
headache, and fever. She had been in her usual state of health until three days prior to admission, when she started cleaning her house with a mixture of household bleach, ammonia, and laundry detergent (same brand as in case 2). After the first day, she developed mucosal irritation, malaise, headache, fevei; and a productive cough. She rested on the second day and felt improved enough to resume her cleaning on the third day. She again noted irritation to her nose, throat, and eyes but continued to work. She produced a small amount of blood-tinged sputum, became progressively dyspneic, and then presented to the hospital. Her past history was noncontributory, and in particular she did not smoke and had no history of asthma or other respiratory disease.
The patient was obese, in marked respiratory distress, with tachypnea, tachycardia, and a pulsus paradoxus. She was afebrile, and her tongue was beefy red. Auscultation of her chest revealed diffuse rhonchi, bibasilar rales, and pronounced wheezing in all lung fields. The heart did not have a gallop rhythm, nor was there any jugular venous distention.
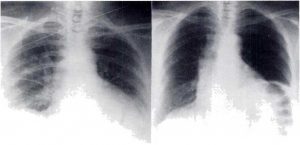
The patient was immediately placed on supplemental oxygen at 5 L/min delivered by nasal cannula. Arterial blood gas determinations on the supplemental oxygen revealed a pH of 7.41, Pa02 of 78 mm Hg (10.3 kPa), and a PaC02 of 36 mm Hg (4.79 kPa). A chest roentgenogram (Fig 3) showed bilateral, patchy infiltrates of the lungs. Her ECG revealed only sinus tachycardia and nonspecific ST changes.
The patient did not relate her cleaning solution to any of her illness except the mucosal irritation, and the history of cleaning with this mixture was not elicited initially by the physician. She was treated with bronchodilators, oxygen, and supportive care. She was given tobramycin and penicillin. When the sputum and blood cultures were negative, the tobramycin was discontinued and the penicillin was continued for seven days. A MUCA scan of her heart revealed a normal left ventricular ejection fraction of 59 percent. Pulmonary function studies on the 12th hospital day revealed a forced vital capacity (FVC) of 1.9 L (59 percent predicted), a forced expiratory volume at one second (FEV) of 1.3 L (53 percent predicted), and a FEV/FVC ratio of 68 percent The total lung capacity was 4.28 L (86 percent predicted).
She gradually improved clinically and was discharged on the 19th hospital day. At discharge, on no supplemental oxygen, her Pa02 was 66 mm Hg (8.78 pka) and PaC02 38 mm Hg (5.05 pka). Nine months after discharge, her Pa02was 79 mm Hg (10.5 pka) and PaC02 36 mm Hg (4.79 pka), but her pulmonary function studies were unchanged. Her chest roentgenogram nine months after discharge (Fig 3) revealed residual diffuse changes, with volume loss and elevation of the left hemidiaphragm. The patient still complained of nonproductive cough and dyspnea on exertion, although this appeared to improve with time.
Figure 1. Admission AP chest roentgenogram (left) taken of the first patient compared with PA film (right) taken 38 days after admission. Residual interstitial infiltrates remained prominent after 38 days.
Figure 2. The second patient had a predominantly interstitial infiltrate on admission AP chest roentgenogram (left) that improved on PA roentgenogram at 21 days (right).
Figure 3. AP roentgenogram of the third patient taken on the day of admission (left) revealed patchy, bilateral infiltrates. PA roentgenogram 9 months later (right) had residual interstitial infiltrates and volume loss on the left.
Category: Pulmonary
Tags: Asthma, dyspnea, respiratory distress, respiratory system